Clock Drawing Test Scoring Numbers Outside Circle
Purpose
The CDT is used to chop-chop assess visuospatial and praxis abilities, and may determine the presence of both attention and executive dysfunctions (Adunsky, Fleissig, Levenkrohn, Arad, & Nov, 2002; Suhr, Grace, Allen, Nadler, & McKenna, 1998; McDowell, & Newell, 1996).
The CDT may be used in addition to other quick screening
tests such as the Mini-Mental State Examination (MMSE), and the Functional Independence Measure (FIM).
In-Depth Review
Purpose of the measure
The CDT is used to apace appraise visuospatial and praxis abilities, and may determine the presence of both attention and executive dysfunctions (Adunsky, Fleissig, Levenkrohn, Arad, & November, 2002; Suhr, Grace, Allen, Nadler, & McKenna, 1998; McDowell & Newell, 1996).
The CDT may be used in addition to other quick screening
tests such as the Mini-Mental Country Examination (MMSE), and the Functional Independence Measure (FIM).
Available versions
The CDT is a simple job completion test in its almost basic class. In that location are several variations to the CDT:
Verbal command:
- Complimentary drawn clock:
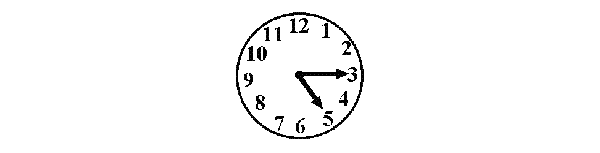
The individual is given a blank sheet of paper and asked first to depict the face of a clock, place the numbers on the clock, and then depict the easily to indicate a given time. To successfully consummate this task, the patient must first draw the profile of the clock, so place the numbers 1 through 12 inside, and finally indicate the correct fourth dimension by drawing in the hands of the clock. - Pre-drawn clock:
Alternatively, some clinicians prefer to provide the individual with a pre-drawn circle and the patient is only required to place the numbers and the hands on the face of the clock. They argue that the patient's ability to fill in the numbers may be adversely affected if the contour is poorly drawn. In this task, if an individual draws a completely normal clock, it is a fast indication that a number of functions are intact. However, a markedly abnormal clock is an important indication that the individual may accept a cerebral deficit, warranting further investigation.
Regardless of which type is used (gratis fatigued or pre-drawn), the verbal command CDT can simultaneously appraise a patient's language function (verbal comprehension); memory function (recall of a visual engram, curt-term storage, and call up of time setting instructions); and executive function. The exact control variation of the CDT is highly sensitive for temporal lobe dysfunction (due to its heavy interest in both memory and language processes) and frontal lobe dysfunction (due to its mediation of executive planning
) (Shah, 2002).
Re-create control:
The individual is given a fully drawn clock with a certain time pre-marked and is asked to replicate the drawing as closely as possible. The successful completion of the copy command requires less employ of linguistic communication and memory functions just requires greater reliance on visuospatial and perceptual processes.
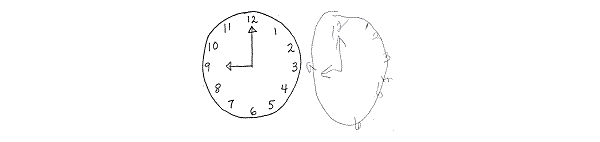
Clock reading test:
A modified version of the copy control CDT simply asks the patient to read aloud the indicated time on a clock drawn by the examiner. The copy command clock-cartoon and clock reading tests are skilful for assessing parietal lobe lesions such every bit those that may result in hemineglect. It is important to do both the verbal command and the copy command tests for every patient as a patient with a temporal lobe lesion may re-create a pre-drawn clock adequately, whereas their clock fatigued to verbal command may prove poor number spacing and incorrect time setting. Conversely, a patient with a parietal lobe lesion may describe an adequate clock to verbal command, while their clock drawing with the re-create command may show obvious signs of neglect.

Time-Setting Instructions:
The most common setting chosen by clinicians is "iii O'clock" (Freedman, Leach, Kaplan, Winocur, Shulman, & Delis, 1994). Although this setting adequately assesses comprehension and motor execution, information technology does not bespeak the presence of any left neglect the patient may have because it does not require the left half of the clock to be used at all. The time setting "x after 11" is an ideal setting (Kaplan, 1988). It forces the patient to attend to the whole clock and requires the recoding of the command "ten" to the number "ii" on the clock. It also has the added advantage of uncovering whatsoever stimulus-bound errors that the patient may make. For case, the presence of the number "10" on the clock may trap some patients and forestall the recoding of the command "10" into the number "2." Instead of drawing the infinitesimal hand towards the number "ii" on the clock to signal "10 afterward," patients prone to stimulus-bound errors volition fixate and draw the minute hand toward the number "ten" on the clock.
Features of the mensurate
Scoring:
There are a number of different ways to score the CDT. In general, the scores are used to evaluate any errors or distortions such every bit neglecting to include numbers, putting numbers in the incorrect identify, or having wrong spacing (McDowell & Newell, 1996). Scoring systems may be unproblematic or complex, quantitative or qualitative in nature. As a quick preliminary screening
tool to simply detect the presence or absenteeism of cognitive damage, you may wish to use a simple quantitative method (Lorentz et al., 2002). However, if a more than complex assessment is required, a qualitative scoring organization would be more telling.
Different scoring methods have been plant to be better suited for different subject field groups (Richardson & Glass, 2002; Heinrik, Solomesh, & Berkman, 2004). In patients with stroke
A psychometric study in patients with stroke
Subscales:
None typically reported.
Equipment:
Only a newspaper and pencil is required. Depending on the method called, you may need to prepare a circle (about 10 cm in bore) on the paper for the patient.
Training:
The CDT can be administered past individuals with little or no training in cognitive cess. Scanlan, Brush, Quijano, & Borson (2002) found that a simple binary rating of clock drawings (normal or abnormal) past untrained raters was surprisingly effective in classifying subjects equally having dementia or non. In this study, a common error of untrained scorers was failure to recognize incorrect spacing of numbers on the clock face as abnormal. By directing at this type of error, cyclopedia between untrained and expert raters should meliorate.
Time:
All variations of the CDT should accept approximately one-2 minutes to complete (Ruchinskas & Curyto, 2003).
Alternative forms of the CDT
The Clock Drawing Exam-Modified and Integrated Arroyo (CDT-MIA) is a 4-pace, twenty-item instrument, with a maximum score of 33. The CDT-MIA emphasizes differential scoring of contour, numbers, hands, and middle. Information technology integrates iii existing CDT's:
- Freedman et al'due south free-drawn clock (1994) on some item definitions
- Scoring techniques adjusted from Paganini-Loma, Clark, Henderson, & Birge (2001)
- Some items borrowed from Royall, Cordes, & Polk (1998) executive CLOX
The CDT-MIA was constitute to be reliable and valid in individuals with dementia, however this mensurate has non been validated in the stroke
Customer suitability
Tin exist used every bit a screening instrument with:
Nigh any patient population (Wagner, Nayak, & Fink, 1995). The examination appears to exist differentially sensitive to some types of affliction processes. Particularly, it has proven to exist clinically useful in differentiating among normal elderly, patients with neurodegenerative or vascular diseases, and those with psychiatric disorders, such as low
and schizophrenia (Dastoor, Schwartz, & Kurzman, 1991; Heinik, Vainer-Benaiah, Lahav, & Drummer, 1997; Lee & Lawlor, 1995; Shulman, Gold, & Cohen, 1993; Spreen & Strauss, 1991; Tracy, De Leon, Doonan, Musciente, Ballas, & Josiassen, 1996; Wagner et al., 1995; Wolf-Klein, Silverstone, Levy, & Brod, 1989).
Can be used with:
- Patients with stroke
Also called a "brain assault" and happens when brain cells die because of inadequate claret menses. xx% of cases are a hemorrhage in the brain acquired by a rupture or leakage from a blood vessel. 80% of cases are as well know as a "schemic stroke", or the germination of a blood clot in a vessel supplying blood to the encephalon. More . Because the CDT requires a nonverbal response, it may exist administered to those with speech difficulties but who have sufficient comprehension to empathize the requirement of the job.
Should non be used in:
- Patients who cannot sympathize spoken or written instructions
- Patients who cannot write
Every bit with many other neuropsychological screening
measures, the CDT is affected by age, education, weather such as visual neglect and hemiparesis, and other factors such equally the presence of depression
(Ruchinskas & Curyto, 2003; Lorentz, Scanlan, & Borson, 2002). The degree to which these factors touch on ones score depends much on the scoring method applied (McDowell & Newell, 1996). Moreover, the CDT focuses on right hemisphere function, so information technology is important to use this test in conjunction with other neuropsychological tests (McDowell & Newell, 1996).
In what languages is the measure bachelor?
The CDT tin be conducted in whatever language. Borson et al. (1999) found that language spoken did not take any direct effect on CDT exam functioning.
Summary
| What does the tool measure out? | Visuospatial and praxis abilities, and may make up one's mind the presence of both attention and executive dysfunctions. |
| What types of clients can the tool be used for? | Virtually any patient population. It has proven to be clinically useful in differentiating among normal elderly, patients with neurodegenerative or vascular diseases, and those with psychiatric disorders, such as depression and schizophrenia. |
| Is this a screening or assessment tool? | Screening |
| Time to administer | All variations of the CDT should take approximately 1-2 minutes to complete. |
| Versions |
|
| Languages | The CDT tin be conducted in any language. |
| Measurement Backdrop | |
| Reliability | Test-retest: Out of four studies examining test-retest reliability , 3 reported splendid test-retest and 1 plant adequate test-retest. Inter-rater: Out of 7 studies examining inter-rater reliability , vi reported excellent inter-rater and ane reported acceptable (for examiner clocks) to fantabulous (for free-fatigued and pre-drawn clocks inter-rater. |
| Validity | Benchmark: Predicted lower functional ability and increased demand for supervision on infirmary discharge; poor concrete ability and longer length of stay in geriatric rehabilitation; activities of daily living at maximal recovery. Construct: The CDT correlated adequately with the Mini-Mental Country Exam and the Functional Independence Measure. Known groups: Significant differences betwixt Alzheimer'south patients and controls detected by CDT. |
| Does the tool detect change in patients? | Not applicable |
| Acceptability | The CDT is brusk and unproblematic. Information technology is a nonverbal task and may be less threatening to patients than responding to a series of questions. |
| Feasibility | The CDT is inexpensive and highly portable. It can be administered in situations in which longer tests would exist impossible or inconvenient. Even the most complex administration and scoring system requires approximately two minutes. Information technology tin can exist administered past individuals with minimal training in cerebral cess. |
| How to obtain the tool? | A pre-drawn circle can be downloaded by clicking on this link: pre-drawn circle |
Psychometric Properties
Overview
Until recently, information on the psychometric backdrop of the CDT were limited. While in that location are many possible ways to administer and score the CDT, the psychometric properties of all the various systems seem consistent and all forms correlate strongly with other cognitive measures (Scanlan et al., 2002; Ruchinskas & Curyto, 2003; McDowell & Newell, 1996). Farther, scoring of the CDT has been found to be both authentic and consistent in patients with stroke
For the purposes of this review, we conducted a literature search to identify all relevant publications on the psychometric properties of the more commonly applied scoring methods of the CDT. Nosotros and so selected to review articles from high impact journals, and from a variety of authors.
Reliability
Test-retest:
Using Spearman rank order correlations of the CDT has been reported by several investigators using a diverseness of scoring systems:
- Manos and Wu (1994) reported an "fantabulous" 2-solar day test-retest reliability
A way of estimating the reliability of a scale in which individuals are administered the same scale on ii different occasions and then the two scores are assessed for consistency. This method of evaluating reliability is advisable only if the miracle that the scale measures is known to exist stable over the interval betwixt assessments. If the phenomenon being measured fluctuates substantially over time, and then the test-retest paradigm may significantly underestimate reliability. In using test-retest reliability, the investigator needs to take into account the possibility of do effects, which can artificially inflate the approximate of reliability (National Multiple Sclerosis Club).
of 0.87 for medical patients and 0.94 for surgical patients. - Tuokko et al. (1992) reported an "adequate" examination-retest reliability
A way of estimating the reliability of a calibration in which individuals are administered the aforementioned calibration on two different occasions and then the two scores are assessed for consistency. This method of evaluating reliability is appropriate only if the miracle that the scale measures is known to be stable over the interval between assessments. If the miracle being measured fluctuates substantially over time, then the test-retest paradigm may significantly underestimate reliability. In using examination-retest reliability, the investigator needs to accept into account the possibility of practice furnishings, which tin artificially inflate the gauge of reliability (National Multiple Sclerosis Society).
of 0.lxx at 4 days. - Mendez et al. (1992) reported and "excellent" coefficients of 0.78 and 0.76 at iii and 6 months, respectively.
- Freedman et al. (1994) reported test-retest reliability
A fashion of estimating the reliability of a scale in which individuals are administered the same scale on ii different occasions and then the two scores are assessed for consistency. This method of evaluating reliability is appropriate only if the miracle that the scale measures is known to be stable over the interval between assessments. If the phenomenon being measured fluctuates substantially over time, then the test-retest paradigm may significantly underestimate reliability. In using test-retest reliability, the investigator needs to take into account the possibility of do furnishings, which can artificially inflate the judge of reliability (National Multiple Sclerosis Society).
as "very low". However, when the "x after 11" time setting was used with the examiner clock, which is known to be a more than sensitive setting for detecting cognitive dysfunction, test-retest reliabilityA manner of estimating the reliability of a scale in which individuals are administered the aforementioned scale on two different occasions and so the two scores are assessed for consistency. This method of evaluating reliability is advisable only if the miracle that the scale measures is known to be stable over the interval between assessments. If the phenomenon being measured fluctuates substantially over time, then the test-retest image may significantly underestimate reliability. In using test-retest reliability, the investigator needs to take into account the possibility of practice effects, which can artificially inflate the estimate of reliability (National Multiple Sclerosis Guild).
was plant to exist "fantabulous" (0.94).
Inter-rater:
Inter-rater reliability
of the CDT, every bit indicated by Spearman rank order correlations (non the preferred method of analyses for assessing inter-rater reliability
but ane used in earlier measurement research), has also been reported by several investigators:
- Sunderland et al. (1989) plant "excellent" coefficients ranging from 0.86 to 0.97 and found no difference betwixt clinician and not-clinician raters (0.84 and 0.86, respectively).
- Rouleau et al. (1992) found "excellent" inter-rater reliability
A method of measuring reliability . Inter-rater reliability determines the extent to which ii or more than raters obtain the same outcome when using the same instrument to measure a concept.
, with coefficients ranging from 0.92 to 0.97. - Mendez et al. (1992) reported "excellent" inter-rater reliability
A method of measuring reliability . Inter-rater reliability determines the extent to which two or more raters obtain the same result when using the same instrument to mensurate a concept.
of 0.94. - Tuokko et al. (1992) reported high coefficients ranging from 0.94 to 0.97 beyond three almanac assessments.
- The modified Shulman calibration (Shulman, Gold, Cohen, & Zucchero, 1993) likewise has "excellent" inter-rater reliability
A method of measuring reliability . Inter-rater reliability determines the extent to which two or more raters obtain the same outcome when using the aforementioned instrument to measure a concept.
(0.94 at baseline, 0.97 at 6 months, and 0.97 at 12 months). - Manos and Wu (1994) obtained "splendid" inter-rater reliability
A method of measuring reliability . Inter-rater reliability determines the extent to which 2 or more raters obtain the same effect when using the same instrument to measure a concept.
coefficients ranging from 0.88 to 0.96. - Freedman et al. (1994) reported coefficients ranging from 0.79 to 0.99 on the free-drawn clocks, 0.84 to 0.85 using the pre-fatigued contours, and 0.63 to 0.74 for the examiner clocks, demonstrating "excellent" inter-rater reliability
A method of measuring reliability . Inter-rater reliability determines the extent to which two or more raters obtain the same result when using the aforementioned instrument to measure a concept.
.
S et al. (2001) compared the psychometrics of 3 different scoring methods of the CDT (Libon revised arrangement; Rouleau rating scale; and Freedman scoring arrangement) in a sample of 20 patients with stroke
were measured using the intraclass correlation coefficient (ICC)
. Raters used similar scoring criteria throughout, demonstrating "first-class" intra-rater reliability
. South et al. (2001) concluded that while the Libon scoring organization demonstrated a range of reliabilities across different domains, the Rouleau and Freedman systems were in the excellent range.
Validity
In a review, Shulman (2000) reported that near studies accomplished sensitivities and specificities of approximately 85% and concluded that the CDT, in conjunction with other widely used tests such as the Mini-Mental Land Exam (MMSE), could provide a significant advance in the early detection of dementia. In contrast, Powlishta et al. (2002) concluded from their written report that the CDT did non appear to exist a useful screening
tool for detecting very mild dementia. Other authors have ended that the CDT should not be used alone equally a dementia screening
test because of its overall inadequate operation (Borson & Brush, 2002; Storey et al., 2001). All the same, nearly of the previous studies were based on relatively minor sample sizes or were undertaken in a clinical setting, and their results may not be applicable to a larger community population.
Nishiwaki et al. (2004) studied the validity
of the CDT in comparing to the MMSE in a large general elderly population (aged 75 years or older). The specificity
of the CDT for detecting moderate-to-severe cognitive harm (MMSE score = 17) were 77% and 87%, respectively, for nurse
administration and 40% and 91%, respectively, for postal administration. The authors conclude that the CDT may have value as a brief face-to-face up screening
tool for moderate/astringent cerebral damage in an older community population but is relatively poor at detecting milder cognitive damage.
Few studies have examined the validity
of the CDT specifically in patients with stroke
coefficients (Pearson correlation
) between the three cognitive tests resulted in r-values ranging from 0.51 to 0.59. Adunsky et al. (2002) ended that they share a reasonable degree of resemblance to each other, bookkeeping for "adequate" concurrent validity
of these tests.
Bailey, Riddoch, and Crome (2000) evaluated a test bombardment for hemineglect in elderly patients with stroke
in the assessment of representational neglect. Farther, consequent with previous findings (Ishiai et al., 1993; Kaplan et al., 1991), the utility of the CDT as a screening
measure out for fail was not supported from these results. Reasons include the subjectivity in scoring, and questionable validity
in that the task may besides reflect cognitive impairment (Freidman, 1991), constructional apraxia, or dumb planning
ability (Kinsella, Packer, Ng, Olver, & Stark, 1995).
Responsiveness
Not applicable.
References
- Adunsky, A., Fleissig, Y., Levenkrohn, Due south., Arad, M., Nov, S.(2002). Clock drawing task, mini-mental state exam and cognitive-functional independence measure: relation to functional outcome of stroke patients. Arch Gerontol Geriatr, 35(2), 153-sixty.
- Bailey, M. J., Riddoch, J., Crome, P. (2002). Evaluation ofa test battery for hemineglect in elderly stroke patients for use by therapists in clinical practise. Neurorehabilitation, 14(3), 139-150.
- Borson, South., Castor, Yard., Gil, E., Scanlan, J., Vitaliano, P.,Chen, J., Cahsman, J., Sta Maria, M. M., Barnhart, R., Roques, J. (1999). The Clock Drawing Test: Utility for dementia detection in multiethnic elders. J Gerontol A Biol Sci Med Sci, 54, M534-forty.
- Dastoor, D. P., Schwartz, G., Kurzman, D. (1991).Clock-drawing: An assessment technique in dementia. Journal of Clinical and Experimental Gerontology, xiii, 69-85.
- Freedman, M., Leach, L., Kaplan, E., Winocur, G., Shulman,Thou. I., Delis, D. C. (1994). Clock Drawing: A Neuropsychological Analysis (pp. 5). New York: Oxford Academy Printing.
- Friedman, P. J. (1991). Clock cartoon in acute stroke.Age and Ageing, 20(2), 140-145.
- Heinik, J., Vainer-Benaiah, Z., Lahav, D., Drummer, D.(1997). Clock drawing exam in elderly schizophrenia patients. International Journal of Geriatric Psychiatry, 12, 653-655.
- Heinik, J., Solomesh, I., Berkman, P. (2004). Correlationbetween the CAMCOG, the MMSE and three clock drawing tests in a specialized outpatient psychogeriatric service. Arch Gerontol Geriatr, 38, 77-84.
- Heinik, J., Solomesh, I., Lin, R., Raikher, B., Goldray, D.,Merdler, C., Kemelman, P. (2004). Clock drawing test-modified and integrated approach (CDT-MIA): Description and preliminary test of its validity and reliability in dementia patients referred to a specialized psychogeriatric setting. J Geriatr Psychiatry Neurol, 17, 73-80.
- Ishiai, S., Sugishita, K., Ichikawa, T., Gono, S., Watabiki,South. (1993). Clock drawing examination and unilateral spatial neglect. Neurology, 43, 106-110.
- Kaplan, E. (1988). A procedure approach to neuropsychologicalassessment. In: T Balderdash & BK Bryant (Eds.), Clinical neuropsychology and brain part: Inquiry, measurement, and practice (pp. 129-167). Washington DC: American Psychological Association.
- Kaplan, R.F., Verfaillie, M., Meadows, M., Caplan, 50.R.,Pessin, M. S., DeWitt L. (1991). Changing attentional demands in left hemispatial neglect. Archives of Neurology, 48, 1263-1267.
- Kinsella, Thousand., Packer, S., Ng, G., Olver, J., Stark, R.(1995). Continuing issues in the assessment of neglect. Neuropsychological Rehabilitation, v, 239-258.
- Lee, H., Lawlor, B. A. (1995). State-dependent nature of theClock Drawing Task in geriatric depression. Journal of the American Geriatrics Gild, 43, 796-798.
- Lorentz, W. J., Scanlan, J. M., Borson, S. (2002). Briefscreening tests for dementia. Can J Psychiatry, 47, 723-733.
- Manos, P. J., Wu, R. (1994). The Ten Point Clock Examination: Aquick screen and grading system for cognitive damage in medical and surgical patients. International Journal of Psychiatry in Medicine, 24, 229-244.
- McDowell, I., Newell, C. (1996). Measuring Wellness. A Guideto Rating Scales and Questionnaires. 2d ed. NewYork: Oxford University Press.
- Mendez, M. F., Ala, T., Underwood, Grand. L. (1992). Developmentof scoring criteria for the clock drawing task in Alzheimers affliction. Journal of the American Elderliness Society, forty, 1095-1099.
- Nishiwaki, Y., Cakewalk, E., Smeeth, 50., Bulpitt, C. J.,Peters, R., Fletcher, A. East. (2004). Validity of the Clock-Drawing Exam equally a Screening Tool for Cognitive Impairment in the Elderly. American Journal of Epidemiology, 160(8), 797-807.
- Paganini-Loma, A., Clark, 50. J., Henderson, V. Westward., Birge, S.J. (2001). Clock drawing: Analysis in a retirement community. J Am Geriatr Soc, 49, 941-947.
- Powlishta, M. K., von Dras, D. D., Stanford, A., Carr D. B.,Tsering, C., Miller, J. P., Morris, J. C. (2002). The Clock Cartoon Test is a poor screen for very mild dementia. Neurology, 59, 898-903.
- Richardson, H. E., Glass, J.North. (2002). A comparison ofscoring protocols on the clock drawing examination in relation to ease of use, diagnostic group and correlations with mini-mental state exam. Journal of the American Geriatrics Lodge, fifty, 169-173.
- Rouleau, I., Salmon, D. P., Butters, N., Kennedy, C.,McGuire, Thou. (1992). Quantitative and qualitative analyses of clock drawings in Alzheimers and Huntington's. Encephalon and Cognition, 18, 70-87.
- Royall, D. R., Cordes, J. A., Polk, M. (1998). CLOX: anexecutive clock drawing task. J Neurol Neurosurg Psychiatry, 64, 588-594.
- Ruchinskas, R. A., Curyto, One thousand. J. (2003). Cerebral screeningin geriatric rehabilitation. Rehabil Psychol, 48, 14-22.
- Scanlan, J. M., Castor, M., Quijano, C., Borson, S. (2002).Comparing clock tests for dementia screening: naïve judgments vs formal systems – what is optimal? International Periodical of Geriatric Psychiatry, 17(1), 14-21.
- Shah, J. (2001). Only time volition tell: Clock cartoon as anearly indicator of neurological dysfunction. P&S Medical Review, 7(2), 30-34.
- Shulman, K. I., Gilded, D. P., Cohen, C. A., Zucchero, C. A.(1993). Clock-cartoon and dementia in the community: A longitudinal study. International Journal of Geriatric Psychiatry, 8(half-dozen), 487-496.
- Shulman, One thousand. I. (2000). Clock-drawing: Is it the idealcognitive screening test? International Journal of Geriatric Psychiatry, xv, 548-561.
- Shulman, G., Shedletsky, R., Silverish, I. (1986). Thechallenge of time: Clock-cartoon and cognitive role in the elderly. International Periodical of Geriatric Psychiatry, i, 135-140.
- South, M. B., Greve, Thousand. Due west., Bianchini, M. J., Adams, D.(2001). Inter-rater reliability of Three Clock Drawing Test scoring systems. Practical Neuropsychology, eight(3), 174-179.
- Spreen, O., Strauss, Eastward. A. (1991). Compendium ofneuropsychological tests: Administration, norms, and commentary. New York: Oxford University Printing.
- Storey, J. E., Rowland, J. T., Basic, D., Conforti, D. A.(2001). A comparison of 5 clock scoring methods using ROC (receiver operating characteristic) curve analysis. Int J Geriatr Psychiatr, sixteen, 394-9.
- Sunderland, T., Hill, J. L., Mellow, A. M., Lowlor, B. A.,Grundersheimer, J., Newhouse, P. A., Grafman, J. H. (1989). Clock cartoon in Alzheimer'south disease: a novel measure of dementia severity. J Am Geriatr Soc, 37(8), 725-729.
- Suhr, J., Grace, J., Allen, J., Nadler, J., McKenna, Thou.(1998). Quantitative and Qualitative Functioning of Stroke Versus Normal Elderly on Half dozen Clock Drawing Systems. Athenaeum of Clinical Neuropsychology, 13(half dozen), 495-502.
- Tracy, J. I., De Leon, J., Doonan, R., Musciente, J.,Ballas, T., Josiassen, R. C. (1996). Clock drawing in schizophrenia. Psychological Reports, 79, 923-928.
- Tuokko, H., Hadjistavropoulos, T., Miller, J. A., Beattie,B. 50. (1992). The Clock Test, a sensitive measure to differentiate normal elderly from those with Alzheimer disease. Periodical of the American Geriatrics Society, twoscore, 579-584.
- Wagner, M. T., Nayak, Thousand., Fink, C. (1995). Bedside screeningof neurocognitive role. In: Fifty. A. Cushman & M. J. Scherer (Eds.), Psychological cess in medical rehabilitation: Measurement and instrumentation in psychology (pp. 145-198). Washington, DC: American Psychological Association.
- Watson, Y. I., Arfken, C. L., Birge, South. J. (1993). Clockcompletion : An objective screening test for dimentia. J Am Geriar Soc, 41(xi), 1235-40.
- Wolf-Klein, Thousand. P., Silverstone, F. A., Levy, A. P., Brod, M.S. (1989). Screening for Alzheimer's disease by clock cartoon.Periodical of the American Elderliness Gild, 37, 730-734.
See the mensurate
Click here to find a pre-drawn circle that tin can be used when administering the CDT.
Source: https://strokengine.ca/en/assessments/clock-drawing-test-cdt/
Belum ada Komentar untuk "Clock Drawing Test Scoring Numbers Outside Circle"
Posting Komentar